A new study has found evidence that a specific brain region could be contributing to some cases of high blood pressure.
And importantly, there may also be a way to reverse it.
According to the study, carried out by a team from the University of São Paulo in Brazil and the University of Auckland in New Zealand, the lateral parafacial (pFL) brain region can trigger biological changes that raise blood pressure.
The pFL is linked to breathing control – specifically those forceful and deliberate exhalations that happen during exercise or when we cough or laugh.
In tests carried out on rats, the researchers found it can also do something else: tighten up blood vessels.
That combination of breath control and blood vessel signaling could be driving hypertension in some cases, the researchers say. It might explain why so many people (around 40 percent by some estimates) still have uncontrolled blood pressure despite taking anti-hypertensive medications.
The study suggests that pFL neurons may link changes in breathing rhythms – which wouldn’t necessarily be noticeable – to increased activity in the sympathetic nervous system (our ‘fight-or-flight’ response) that helps control blood pressure, fitting with previous research that has linked hypertension to the brain and nervous system.
“Given that around 50 percent of patients with hypertension have a neurogenic component, the challenge is to understand mechanisms generating sympatho-excitation in hypertension,” write the researchers in their published paper.
“Such a revelation would provide much-needed clinical orientation for new therapeutic strategies.”
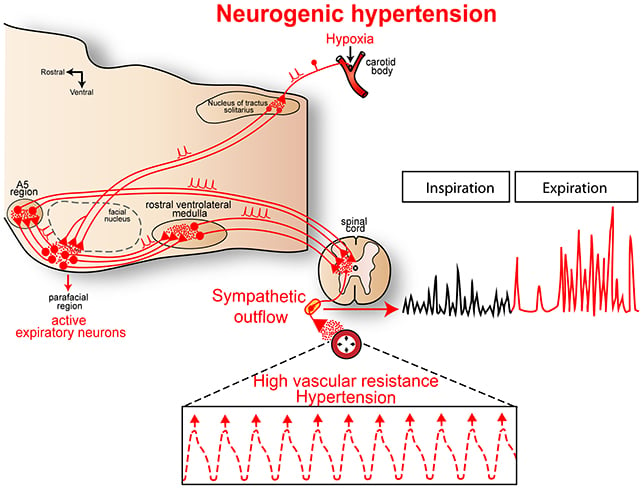
In their experiments in rats, the researchers used genetic engineering techniques to turn pFL neurons on or off, then observed the effects. Breathing-related nerve activity, sympathetic nerve activity, and blood pressure were all monitored.
The researchers activated pFL neurons in some rats, and found this triggered other brain circuits that ultimately raised the animals’ blood pressure.
They were then able to map out brainstem and nerve activity in detail, including the other neurons that the pFL region was communicating with, and compare it with readings from control rats without hypertension.
In hypertensive rats, pFL neurons weren’t just helping with breathing, but also acting to constrict blood vessels. The finding also revealed a new potential treatment pathway.
“We discovered that, in conditions of high blood pressure, the lateral parafacial region is activated and, when our team inactivated this region, blood pressure fell to normal levels,” says physiologist Julian Paton, from the University of Auckland.
The findings published here also go some way to explaining why people who have sleep apnea – problems breathing in the night – also have a higher risk of high blood pressure.
It’s that connection between breathing and blood flow again: While pFL neurons aren’t involved in normal breathing, they fire up in response to high CO2 or low oxygen levels, which is what happens during sleep apnea.
It’s important to acknowledge that this research only used animal models – it’s likely but not certain that the same circuitry is involved in people too.
However, with around a third of the global population thought to have a problem with high blood pressure – and many of those unable to access medication that can help – the need for new treatment options is an urgent one. Hypertension seriously increases the risk of many heart issues and has been linked to multiple other conditions, such as dementia.
Related: Study Reveals How Much Exercise You Need Weekly To Control Blood Pressure
The next challenge is figuring out how drugs might be able to target the pFL neurons in particular, without interfering with anything else – and the researchers report that they’ve made some headway here too.
Carotid bodies are clusters of cells that act like tiny sensors in the neck, and can influence pFL neurons from outside the brain. The researchers believe that targeting these sensors might be enough to keep the pFL region in check.
“Our goal is to target the carotid bodies, and we are importing a new drug that is being repurposed by us to quench carotid body activity and inactivate remotely the lateral parafacial region safely, i.e., without needing to use a drug that penetrates the brain,” says Paton.
While this strategy might seem easier than getting a drug to penetrate the brain, it will still require extensive testing.
The research has been published in Circulation Research.

